
Rural doctors are welcoming a federal government review into the distribution of health professionals across Australia, but say there won't be a quick fix to improve access for rural and remote communities.
Subscribe now for unlimited access to all our agricultural news
across the nation
or signup to continue reading
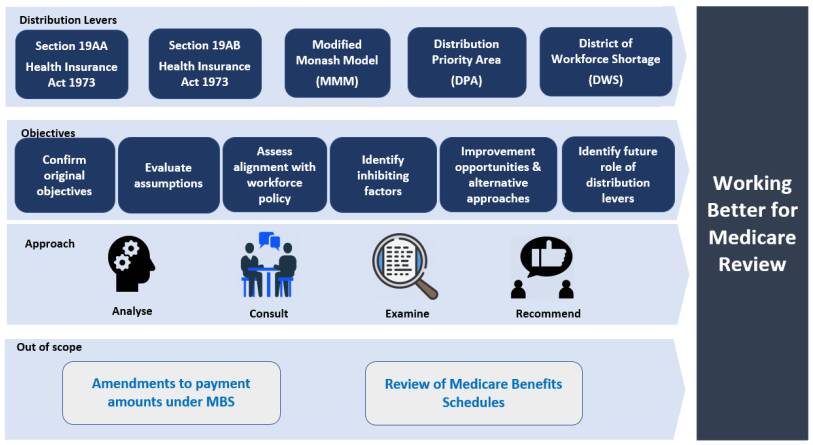
The Working Better for Medicare review will look into the policies which are currently used to encourage staff to work in the areas where they're needed most, such as laws governing when overseas-trained doctors can access Medicare benefits.
Workforce classification schemes are also in the spotlight, such as Distribution Priority Areas (DPA), which identify regions with GP shortages, and the Modified Monash Model (MMM), which classifies regions on a scale from metropolitan to remote.
Rural Doctors Association of Australia president Dr RT Lewandowski said the schemes were important levers, but needed to be targeted to be effective.
"Doctors who have a requirement in DPAs to tend to shift closer and closer to urban centres when the requirements change," Dr Lewandowski said.
"Recently there was a change when Modified Monash 2, which is just out of regional places, became DPAs, and we did see a number of GPs who were working more regionally and remotely move back into the city.
"We know that does have an effect, particularly on international medical graduates and on people who have bonded scholarships from the government."
While the RDAA is wary of any move to replace the MMM, the Australian College of Rural and Remote Medicine (ACRRM) argues the data unpinning the original model is due for an update.
ACRRM president Dr Dan Halliday said the demographics of Australia's medical workforce had also changed.
"A significant part of that is that due to COVID we've actually seen a greater resignation of general practitioners out of the workforce and early retirements," Dr Halliday said.
"We've actually seen a significant reduction in the migration patterns of medical practitioners into Australia.
"Our international medical graduates that would normally come into Australia to assist with our workforce needs haven't been there."
The RDAA and ACRRM are likely to be engaged alongside other key stakeholders as part of the review, with the government expecting to receive the findings in mid-2024.
An external consultant will be appointed to conduct the review, while rural health expert Professor Sabina Knight and former health bureaucrat Adjunct Professor Mick Reid will independently oversee the process.
The announcement comes amid public consultation to recognise rural generalism as a specialist field within general practice and growing concern the health system is out of touch with the regions.
Dr Lewandowksi said it would take more than incentives to solve the issue, but a broader effort to develop the medical workforce outside of urban centres and large hospitals.
"Ideally, we'd also be looking at ways to find doctors and health practitioners who choose a really good career in rural and remote health, without levers that kind of force them to be there," Dr Lewandowski said.
"We're going to have to look at the entire pathway - how we start, how we recruit, how we train, and then of course, the incentives and levers at the end.


